restorative Medicine
Restoring Hand Function in People With Complete Spinal Cord Injury
A clinical study underway at Houston Methodist indicates that a nerve transfer surgery will allow spinal cord injury patients to move their hands 50% of the time.
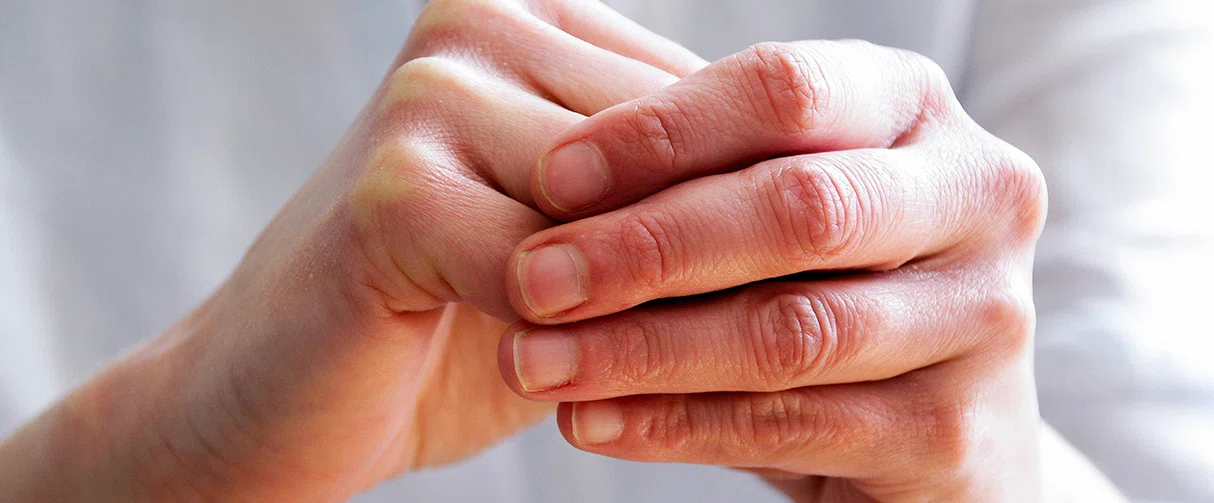
Spinal cord injuries’ devastating consequences rob a person’s physical and mental well-being. To improve the quality of life for those afflicted by spinal trauma, peripheral nerve transfers are a line of treatment that could restore some of the lost function in the muscles once receiving innervation from the injured portion of the spinal cord.
At Houston Methodist, Amir Faraji, MD, PhD, assistant professor of neurological surgery, is one of the principal investigators of a multicenter clinical study to evaluate the outcomes a nerve transfer surgery on patients who have lost their arm and hand function from a complete spinal cord injury. Currently, Houston Methodist is the only site in the southern United States that is enrolling patients for this Department of Defense-funded, multicenter clinical trial.

Amir Faraji, MD, PhD
Assistant Professor of Neurosurgery at Houston Methodist
“This project stemmed from my interest in treating spinal cord injury patients, which is an area that Houston Methodist has a history in for many years,” said Faraji.
Spinal cord injuries affect roughly one in every 1000 people in the United States and could be caused by falls, vehicle accidents and infections, among other reasons. In addition to the physiological and medical impacts, the injury poses a huge psychological burden due to the lack of functional independence, which deeply impacts an individual’s daily life. Thus, recovering some of the lost muscular functions due to the injury has been an active area of clinical intervention.
Among the available surgical options, tendon and peripheral nerve transfers have carved out a space for treating spinal cord injuries. A tendon transfer is an orthopedic procedure where a working tendon is moved to a muscle whose function is lost. So, for example, if the hand function is lost, a working tendon from the arm is cut and reconnected to the hand. Faraji said although the procedure could be done at any time after the injury, fine hand movements will still be lacking.
This limitation of tendon transfers, however, could be overcome with nerve transfers. In this procedure, a donor nerve originating from above the injury site in the spinal cord is transferred into a recipient nerve conduit in the arm that comes from below the injury. Faraji and his team’s study tests the efficacy of nerve transfers in patients that have little to no arm and hand function due to complete spinal cord injury.
A scientific illustration of a nerve transfer surgery for restoring hand movements. Here, a branch of the musculocutaneous nerve to the brachialis muscle is the donor nerve and the anterior interosseous nerve (AIN) is the recipient nerve. Image designed by Rachel Whitehead.
For their clinical trial, the researchers included patients between 18 and 65 years of age who have sustained a traumatic injury to the C4-C8 region of the spinal cord at most 36 months ago. These candidates also have little to no use of their hands and have received at least three months of non-operative rehabilitation therapy. Prior to the nerve transfer, the patients receive preoperative electromyography and nerve conduction evaluations to ensure that the donor and recipient nerves are viable for nerve transfer. Most notably, if the patients are planning on undergoing a tendon transfer during the study period or have had a tendon transfer in the past, they are excluded from the clinical trial.
Although their study is still underway, Faraji noted that they have promising evidence that it is successful in allowing meaningful hand movements around 50% of the time. Further, the clinical study also keeps patients in occupational therapy so that the nerves are encouraged to grow toward their muscle target.
Faraji noted that one of the main goals of the study is to better define the patient outcomes after the nerve transfer. With this information in hand, the surgical procedure could be optimized even further by using growth factors to promote nerve growth or electrical stimulation to jumpstart nerve function.
“The recovery from nerve transfers is slow and won’t restore the lost movement completely, but it will certainly improve quality of life vastly,” said Faraji. “If the surgery helps our patients hold a toothbrush to brush their teeth or grab their cellphones better, it goes a long way in improving their functional independence.”
Vandana Suresh, PhD
September 2022
Related Articles