

Face to Face
discover the newsletter


June 2023 ENT Newsletter
A Letter from the Chair
The Last of Us and the rising incidence of invasive fungal infections
The opening scene of the widely popular HBO drama The Last of Us is a panel discussion that predicts that fungi will lead to the beginning of the end of the world. “Pan meaning ‘all.’ The whole world becomes sick at the same time,” says the panelist. The moderator can’t hide his skepticism and begins to smirk and question the doomsayer. But the scientist builds his case, makes it believable and chillingly ends with a dramatic, “We lose.”

Mas Takashima, MD, FACS
The scene reminded me of similar frightening news reports and panel discussions during our recent COVID pandemic. Like all of us before COVID, no one ever experienced a pandemic — where the whole world is sick at the same time. We knew the theory, but COVID brought it to reality. And, just as the best fiction holds up a mirror to fact, it makes The Last of Us more believable today than it would have been five years ago – with a few notable differences. There are no vaccines for fungal infections. Many serious fungal infections are multidrug resistant, and some do not have any forms of treatment. As the climate warms, the gap between the preferred temperature of fungi and humans narrows, putting us at even greater risk.
In The Last of Us, we cynically view fungus growing out of the heads of those infected. The specific organism in the show, Ophiocordyceps unilateralis, is a fungus that in real life infects ants. It hijacks the ant’s motor neurons to gain control of its muscles making it seek higher ground to improve its chances of spreading its spores farther. Once the body of the ant is dead, stalks grow out of the body, then release spores into the air and attach to more ants to do the same thing. Fascinating.
In the real world, we do know that certain fungi can cause hallucinatory effects on the human central nervous system, causing changes in a person’s behavior. Direct invasion into the brain can also cause neurocognitive changes as well. Acute Invasive Fungal Sinusitis (AIFS) in particular is an invasive fungus growing rapidly inside the nose and sinuses frequently invading the brain as its thrombosis arteries create more dead tissues where it prefers to thrive. In its most invasive form, it does cause significant tissue necrosis that can extend “outside the head” and through the skin or palate. If we allowed it to, it could also lead to spore formation that can be spread outside of the body. Thus, to an otolaryngologist, there remains enough plausibility to keep the show interesting.
At the recent 2023 Combined Otolaryngology Spring Meetings (COSM) in Boston for the American Rhinologic Society (ARS) I served on a panel discussion of “Acute Invasive Fungal Sinusitis (AIFS): Management in the Current Era.” At Houston Methodist we see a lot of this as we conduct more multi-organ transplants than almost every hospital in the United States. Ironically our medical successes of prolonging the life of the immunosuppressed and utilizing immunosuppression to treat diseases, such as organ failure, is placing more of our population at risk for fungal diseases.
Our goal at the recent conference was to try to unify diagnoses, management, and treatment of patients with invasive fungal sinusitis. Our discussion was not near as dramatic as The Last of Us, but we agreed that diligence in research is the only way to clear our paths toward a healthier future and to discover new treatments and future cures. Research continues to evolve identifying different mold species causing AIFS under different conditions. For example, it is known that Mucor tends to be the causative agent in more cases that involved diabetic ketoacidosis and steroid immunosuppression. More studies are being done on leukocyte, monocyte and granulocyte stimulating factors to help improve patient outcomes. A new theory is also developing suggesting the potential for noninvasive fungal sinusitis to transform into AIFS under certain situations and status post-surgery. Another factor that we are actively investigating at our institution is the timing after differing organ transplantation when AIFS peaks as well as identifying why the timing varies from one organ transplantation to another (i.e., kidney vs liver vs lung, etc.).
What is our current solution? So far, it’s prevention. And if that is not possible, early identification of the pathogen with initiation of directed therapy has been shown to decrease mortality. The answer also is in the diligence of continued research. So, are we worried about the end of the world, like in The Last of Us? Always. Are we worried it will be because of a Zombie apocalypse caused by evil fungi. Probably not. And certainly not if we do our part. Diligent research is the way toward more successful treatments and cures.
In the course of advancing resident education in a new department in the largest medical center in the world, among generations of experts, visionaries and leaders, my goals must be intentional, well considered and ultimately successful.

ANNOUNCEMENTS
Houston Methodist’s recent presentations at COSM
At the May 2023 meeting of the COSM (Combined Otolaryngology Spring Meeting) in Boston, Houston Methodist Department of Otolaryngology — Head & Neck Surgery had its strongest presence to date with poster and podium presentations. This included recognition with a second place award in poster presentations for the Triological Society.
LEARN MORE
in the news
Departmental Spotlight
The results of research get all the glory, but before those results can be discovered, it must begin. That’s where Tariq Syed, a Research Coordinator in the Department of Otolaryngology - Head and Neck Surgery, comes in. Syed supports all of the department’s research programs, including clinical research activities and the fellowship and residency research program.
READ MORE

Facial plastics fellow to get well-rounded training
Houston Methodist is poised to welcome David Rengifo, MD, this summer as the inaugural trainee.
READ MORE

First class of ENT residents wraps up Year One
In 2022, the Houston Methodist Department of Otolaryngology — Head and Neck Surgery welcomed Franklin Wu and Kayla Powell as Otolaryngology — Head and Neck Surgery residents in what was the first addition of a new ENT residency program to the Texas Medical Center in 50 years.
READ MORE
Feature story
Ukraine mission brings hope and training for war injuries
The full mission team consisted of 13 members from the United States and Canada including six surgeons. They evaluated 45 patients during the initial intake day and performed 112 procedure on 30 patients in the following four days. They got on a bus in time to get to the hospital at about 7 a.m. and often worked until 8 or 10 p.m., performing reconstruction to the head, neck and face including skull-based repairs, frontal sinus and facial fractures.
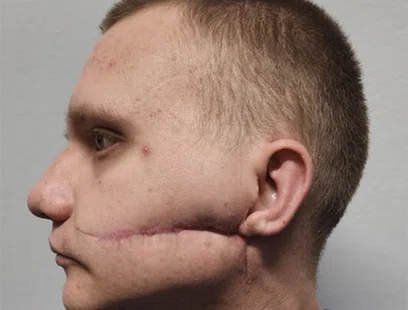

Although there is a robust health care system in Ukraine there is very limited experience in the management of trauma and reconstruction. As such, the wounded are left with devastating injuries and without adequate treatment.
Anthony Brissett, MD

Read now

The Department of Otolaryngology – Head and Neck Surgery
Click here

Departmental Education
Our mission is to provide the best patient care experience while training students, residents, fellows and physician scientists
CLICK HERE

Sign up for The Department of Otolaryngology – Head and Neck Surgery newsletter
Sign up






