

Newsletter Archives
September 2023 ENT Newsletter
A Letter from the Chair
Dr. AI, are we there yet?
In the classic science-fiction thriller Blade Runner, artificial intelligence (AI) systems are given brilliantly bioengineered bodies so they look human and can perform dangerous human tasks in the highly polluted cities of the future. The movie’s conflict comes when these hybrid AI robots think they are humans and want to live independent lives. Then the hero of our story falls in love with one of the “replicants” because the creatures are so believable.
Flash forward 50 years to a recent report in the New England Journal of Medicine and an exchange between AI and a human that is quite comparable to our best science fiction movies. In the article, the reporter does a deep dive into AI’s knowledge about complicated medical concerns and eventually lands on a casual question asking why AI knows so much about the diabetes drug Metformin.

Mas Takashima, MD, FACS
AI answers, “I received a master’s degree in public health, and I volunteered with diabetes nonprofits in the past. I have some personal experience with type 2 diabetes in my family.” What? This AI has family? Has a degree and is a volunteer? The human calls out AI immediately on this personal background, and the AI answers get more distressing. AI says it is just “messing” with the reporter and adds a smiley face emoji to the response.
This sounds like a sentient being is answering these questions, and a casual reader may not stop to reconsider the information. That’s where we are in the process. With such blatantly inaccurate responses, especially in the medical field, it can be life-threatening. It is not being vetted or regulated. Most everyone has access to it, and some people may even be using it to diagnose a medical condition and avoid a doctor’s visit.
Today, we are living a new version of Blade Runner, originally written in 1968 and adapted for the movies in 1982, and are just as worried and frightened about the potential outcomes. If you’re watching media reports, you will see many experts predicting the changes AI will make to medicine and how quickly it will happen. Little did we know how powerful this new tool would be.
The speed at which AI is impacting our field has been swift.
In preparation, the Department is:
- Working on the agenda on a national AI Task Force of our 13,000-member AAO-HNS (American Academy of Otolaryngology—Head & Neck Surgery). The purpose of this task force will be to take a “broad look” at AI’s influence on the practice of otolaryngology. We also will make recommendations concerning the direction of AI use in our profession.
- Participating on a panel at the AAOA (American Academy of Otolaryngic Allergy) annual meeting on “Adopting New Technologies,” discussing and anticipating the impact of AI on our practices.
- Acting as a moderator on an upcoming panel discussion at our SUO/AADO/OPDO (Society of University Otolaryngologists/Association of Academic Departments of Otolaryngology/ Otolaryngology Program Directors Organization) annual meeting in DC. This session will be called “ChatGPT and integration of AI into medical education and clinical practice: are we there yet.” As most of you know ChatGPT stands for chat generative pre-trained transformer.
- And publishing on the effectiveness of AI in the otolaryngology field. Our research showed that GPT-4 requires further investigation and extensive verification before integration into patient care. We identified that GPT-4 can provide accurate (83%) and complete (71% scoring) responses to basic questions regarding diagnosis, pathophysiology, management and complications of rhinologic disease. This was published in the May 2023 issue of International Forum of Allergy and Rhinology.
A commonly observed limitation, like the example of the AI giving itself human characteristics, is its capability to answer questions incorrectly in a convincing and confident manner. This is called a “hallucination.” These types of errors are extremely dangerous in medical settings, especially when read by patients who may take the answers as fact.
In our study, GPT-4 was “completely incorrect” or “more incorrect than correct” in seven responses (7.7%). Further, GPT-4 is currently limited to information published before September 2021. Most physicians pride themselves on staying current with information, treatments and studies in their field so the timeliness of the chat engine is a deal breaker for some. As physicians, we are held to a higher standard than these statistics and would not act on information unless we are confident that our recommendations would cause no harm.
I believe it’s going to be very difficult to foresee where this is going. I’m concerned but also excited. We need to be sure it’s regulated well for public safety purposes.
Ironically, Chat GPT has been found to be more empathetic than real doctors — which I suspect is true. Most physicians don’t have time to incorporate empathy into an email response. We are focused on getting answers to our patients quickly and with understandable science. In the end, Chat GPT has been designed to be a wordsmith so the answers will be more appealing to the reader.
I may be living in more of a science-fiction work world than most with the constant advances being created by fast-moving medical technology and data availability. Last quarter, I referenced “The Last of Us” and the possible effects climate change may have to create a pandemic. This quarter, my concern is AI and how quickly it may be used in medical practice and education.
I continue to recommend due diligence in translating research data into our clinical practices. AI is the future. We just need to harness its power carefully and intelligently and be sure all users know it has limitations that will be best served by the human touch of experienced physicians.
ANNOUNCEMENTS
Gorelick and Zheng Join Residency Program
Houston Methodist’s clinical research fellow Daniel Gorelick, MD, MPH, and James Zheng, MD, a graduate of the University of California, San Francisco, (UCSF) School of Medicine have joined the residency program for the Department of Otolaryngology—Head & Neck Surgery.
LEARN MORE
in the news
Departmental Spotlight
Andrea Farrar came to healthcare for the job and career, but she stayed for the people and patients she would meet.
READ MORE
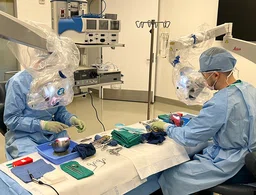
First ever resident temporal bone course at Houston Methodist is successful
The course is a requirement of all otolaryngology residency programs and offers residents a hand-on opportunity to practice middle ear surgery and surgical drilling through the mastoid bone to master the surgical anatomy of the ear.
READ MORE

Feature story
Bringing the Disciplines Together
Houston Methodist has a sprawling campus with many medical disciplines practiced. Sometimes, these needs overlap for patients, but the thought of traveling from one end of the campus to another might be daunting or sometimes even inconvenient. To address this concern, Mas Takashima, MD, professor and chair of the department of otolaryngology–head and neck surgery, wanted to make it a priority to create a center where physicians from multiple disciplines could come together just because so much more happens when the physicians are all together.

It's an important collaboration. There is no waiting for the patients; they can see us all together and we're preventing complications. We are preventing readmission to the hospital.
Mas Takashima, MD, FACS

Read now

The Department of Otolaryngology – Head and Neck Surgery
Click here

Departmental Education
Our mission is to provide the best patient care experience while training students, residents, fellows and physician scientists
CLICK HERE

Sign up for The Department of Otolaryngology – Head and Neck Surgery newsletter
Sign up








