Biomimetic nano drug delivery carriers for treating cardiovascular diseases (CVD) hold a great therapeutic potential by mimicking the way circulating cells in our body behave during these diseases.
Someone in the United States dies from cardiovascular diseases every 37 seconds despite improved medical therapies and a well-defined understanding of the disease progression. The outcomes for many CVD patients could be further improved with updated drug delivery mechanisms that circumvent the inherent limitations of traditional systemic delivery of free drugs. These shortfalls include the biological challenges of short systemic circulation time and off-target toxic effects as well as physiochemical issues with inadequate levels of drug in the target tissue and poor solubility.

Someone in the
United States dies
from cardiovascular
disease every
37
seconds
For the last 30 years, this need has motivated scientists around the world to improve the effectiveness of pharmacotherapies. For instance, synthetic drug carriers are being developed to further enhance the selectivity, effectiveness and safety of existing drugs. They also have the potential to solve delivery and stability challenges that accompany novel classes of drugs such as RNA therapeutics.
Nanotechnology represents a powerful tool for meeting the unsolved needs of clinical drug delivery, offering a broad range of synthetic nanoparticles in the form of liposomes, micelles, polymeric spheres among others, that are designed specifically to target diseased tissues. Although there are not yet any clinically available nanoparticles for treating CVD, they are currently used in clinical practice for the treatment of respiratory distress syndrome, certain types of cancer such as breast and pancreatic and some genetic diseases like hemophilia. However, upon systemic administration, these nanoparticles encounter several biological barriers that prevent them from optimally fulfilling their therapeutic task.
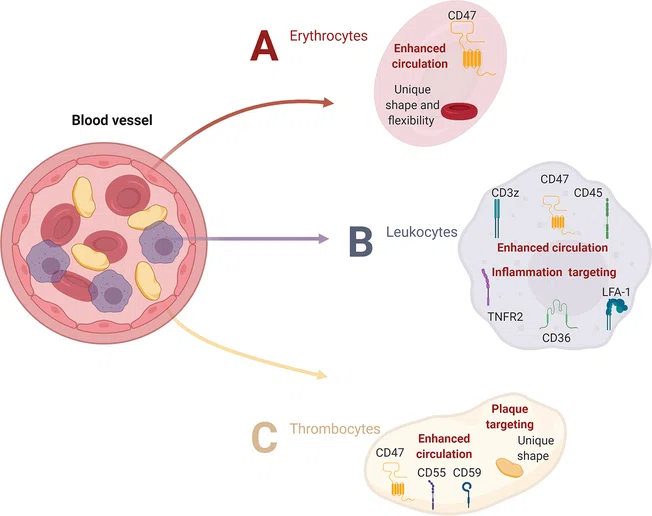
Native cells and their inherent functional moieties, which allow the native cells to evade the biological barriers and reach the target. All the proteins in this figure are membrane proteins and were placed inside the cells only for visualization.
Inspired by the way cells in our body respond to CVD pathologies, biomimetic nanoparticles hold great promise. Progress in biomimetic nanoparticle engineering design principles, including surface engineering and morphology engineering, will advance this field to discover novel, exciting therapeutic solutions.

Francesca Taraballi, PhD
Assistant Professor of Orthopedic Surgery
Director, Center for Musculoskeletal Regeneration
Houston Methodist
Looking forward, there are numerous opportunities for treating CVD using biomimetic nanoparticle technologies. Novel therapeutic agents that have already demonstrated pre-clinical efficacy in treating CVD, such as miRNA and CRISPR/Cas9, can be encapsulated in these platforms. Patient specific, personalized treatments made using the patient's own cells can be fabricated in the future to increase these platforms' biocompatibility profiles. In addition, gaining a better understanding of the biological underpinnings of CVD development will allow scientists to target specific mechanisms and disease stages to improve therapeutic outcomes.
The solution is far from straightforward and a panoply of solutions have been explored. In a recent review published in Nanomedicine: Nanotechnology, Biology and Medicine, Houston Methodist’s Assaf Zinger, PhD, postdoctoral fellow, John Cooke, MD, PhD, Director of the Center for Cardiovascular Regeneration and Francesca Taraballi, PhD, Director of the Center for Musculoskeletal Regeneration discuss how biomimetic nano drug delivery carrier systems, inspired by the way different cells in our body respond to CVD pathologies, may hold great therapeutic potential in addressing the challenges posed by biological barriers.
Biomimetic nanoparticles aim to subvert biological barriers by mimicking native cells either through the bioengineering of the nanoparticular surface or by imitating the complex morphology of native cells. Most biomimetic nanoparticles for CVD treatment have been engineered to target activated endothelia that occur when inflammation is present. This form of endotheliopathy is a common denominator in different stages of CVD pathophysiology. Other approaches exploit the shape of circulating cells to allow higher oxygen binding and improved access to the microvasculature, which may be useful in treating CVD.
Promising as it sounds, this natural cell-inspired biomimetic nanoparticle technology still needs to overcome cell-specific and general roadblocks before it can be used in clinical practice. For instance, current synthetic nanoparticle systems lack active disease targeting, have shorter systemic circulation times compared to native circulating cells and can trigger an immune response. In addition, various scientific questions still need to be answered before clinical utilization. First, batch to batch reproducibility should be assessed. Second, contamination of the biomimetic nanoparticles by other plasma membrane components needs to be characterized and controlled. Finally, scientists must complete the studies needed to better understand the scale-up feasibility of these platforms.
Zinger A, Cooke JP, Taraballi, F. Biomimetic nano drug delivery carriers for treating cardiovascular diseases. Nanomedicine: Nanotechnology, Biology and Medicine: April 1, 2021. DOI: https://doi.org/10.1016/j.nano.2021.102360
Donna Ostermayer, December 2021
Related Articles

Precision Medicine
Nano Doses Delivered in Space
Study explores potential biomedical applications at the ISS
PRECISION MEDICINE
RNA therapeutics have the potential to transform standard patient care and actualize personalized medicine
RNA as a therapeutic molecule holds great power and the potential to alter the standard of care for patients, actualize personalized medicine, and have diverse applications.